GUEST BLOG: How high does vaccination coverage need to be to establish herd immunity?
11.03.2021In the Rokotustieto.fi guest blog, Mika Rämet, Director of Tampere University’s Vaccine Research Center, explains the factors that have an impact on establishing a vaccination coverage that is sufficient to achieve herd immunity.
I am often asked how high vaccination coverage should be in order to establish herd immunity. I dodge the question just as often by saying that there is no precise figure to give. The higher the vaccination coverage, the easier it is to suppress an epidemic.
Restrictions are the only way to curb an epidemic until we achieve herd immunity
Herd immunity means that there is a sufficient number of people in the population who are resistant to a disease to ensure that those who are not resistant can also avoid becoming ill. In Finland, for example, the vaccination coverage of the MMR vaccination, which protects against measles, mumps and rubella, is so good that even those who have not received the vaccination are quite well protected.
To establish herd immunity against the coronavirus a sufficient proportion of the population must be immune, in other words resistant, to the disease-causing SARS-CoV-2 virus, either as a result of having had the diseases or having received an effective vaccine. Until the vaccine is in widespread use, the exponential growth in the number of cases can be prevented by limiting the number contacts of those with the virus (quarantines, remote work and remote school, restrictions on gatherings, social distancing and restrictions on movement) and reducing the risk of infections in contact situations (face masks and good hand and cough hygiene). The aim of these extremely important measures is to curb the epidemic and to protect people belonging to risk groups until an effective vaccine is available for widespread use.
It is worth bearing in mind that infection is also possible even if you conscientiously observe the safety guidelines. If the measures are insufficient and people do not behave responsibly, the epidemic will begin to spread at an accelerating rate. Restrictions will slow it down, but ultimately only a vaccine will prevent the epidemic from spreading across the entire population.
Vaccinations will not have a strong impact on the epidemic to begin with
Covid-19 vaccinations were started in Finland in late December 2020. Initially, the specific benefit of the vaccines is that they provide very good protection against Covid-19, including the severe forms of disease. In other words, by being vaccinated, you protect yourself. If you remain healthy, you will help to protect medical care capacity and thus help others.
Vaccination will initially have a rather minor impact on the epidemic. A large proportion of the population is still vulnerable to the virus and even those who have been vaccinated can still spread the disease. We must therefore continue to curb the epidemic by means of restrictive and protective measures, otherwise it will accelerate as illustrated by Figure 1.
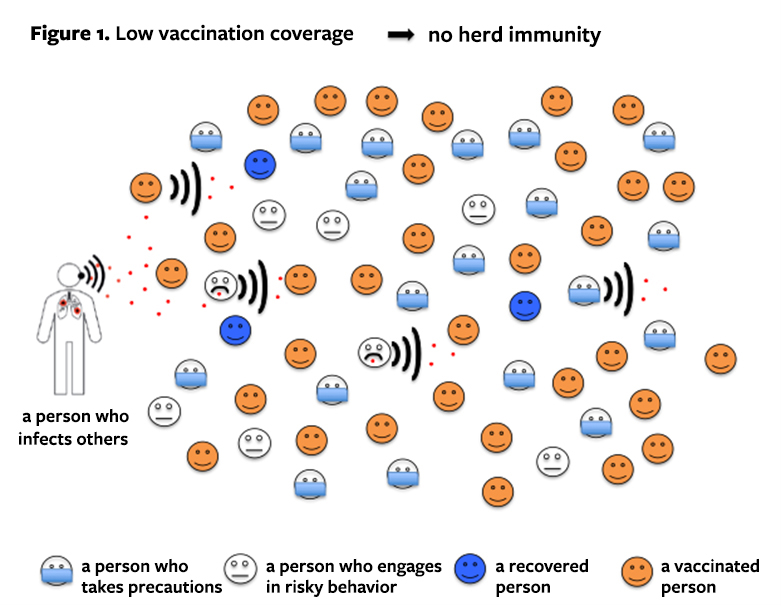
If the vaccinations are successfully aimed, the first observed effect should be a reduction in mortality after the people most at risk of a difficult disease have been vaccinated. Vaccinating healthcare workers secures hospitals’ ability to operate.
It is not yet possible to determine sufficient vaccination coverage
Extinguishing the epidemic requires high vaccination coverage and the responsible behaviour of those who have been vaccinated (Figure 2).
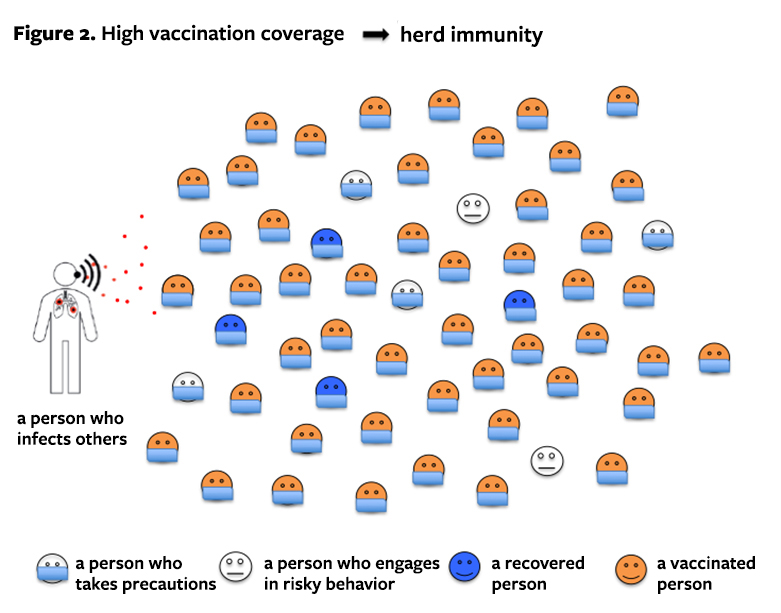
The vaccination coverage regarding Covid-19 can be considered adequate when the basic reproduction number remains below one. This means that the epidemic will not spread. In practice, this means that an infected person causes less than one new case of the disease on average. This depends on the number of contacts of the infected person has and how likely transmission is in contacts between people. The lower the risk, the lower the need to restrict contacts. But if the mathematics used to calculate a sufficient vaccination coverage is not difficult, why am I unwilling to give clear figure?
Many factors that are still uncertain influence the determination of sufficient vaccination coverage to establish herd immunity:
- How much will vaccination reduce infectiousness? Several different Covid-19 vaccines are being used, with potentially differing effects on infectiousness.
- The impact of vaccination on the spread of the epidemic varies between age groups and regions. In terms of the epidemic, good vaccination coverage is particularly important in the age groups with the highest number of contacts. Correspondingly, vaccination coverage should be particularly good in areas where the number of cases is high.
- How successful will we be in restricting contacts? The fewer the contacts between humans, the smaller the proportion of the population that needs to be immune to the disease (either due to previous exposure, existing resistance or vaccination). This, in turn, is influenced by how strict the restrictions imposed are and how they are targeted (geographical area, age class, etc.).
- How committed will vaccinated and non-vaccinated people be to observing restrictive and protective measures? This affects how likely the disease is to be transmitted in the event of a contact. Human behaviour is difficult to predict and depends on how relevant the restrictive measures are felt to be.
- How will the epidemic behave? The epidemic may well ease off in the summer, as was the case in 2020.
- How much of the population will have been exposed to the virus by the summer, and will there be a high level of natural resistance to the virus in the population?
Significant vaccination coverage is required for the epidemic to die out. Therefore, there is no point in putting our trust in herd immunity for a long time yet. However, the larger the number of people vaccinated, the easier it will be to loosen restrictions. When the majority of the adult population has been vaccinated and, at the same time, we remember to act responsibly towards others, we will succeed in eradicating the coronavirus epidemic.

Mika Rämet
Professor of Paediatrics and Experimental Immunology
